The Heartbreak Connection: How Bereavement Increases Cardiovascular Risk
Losing a loved one is one of the most taxing emotional experiences a human can endure. While the psychological toll of grief is well-documented, the physical impact on the heart is equally profound. Recent research indicates that bereavement—the period of mourning after a death—is linked to a significantly higher risk of cardiovascular disease (CVD), a connection that became even more pronounced during the COVID-19 pandemic.
Understanding this link isn’t just about acknowledging emotional pain. it’s about identifying a critical window of physiological vulnerability. For those grieving, the heart may be at a higher risk for acute events, necessitating targeted medical monitoring and proactive wellness strategies.
The Science of Grief and the Heart
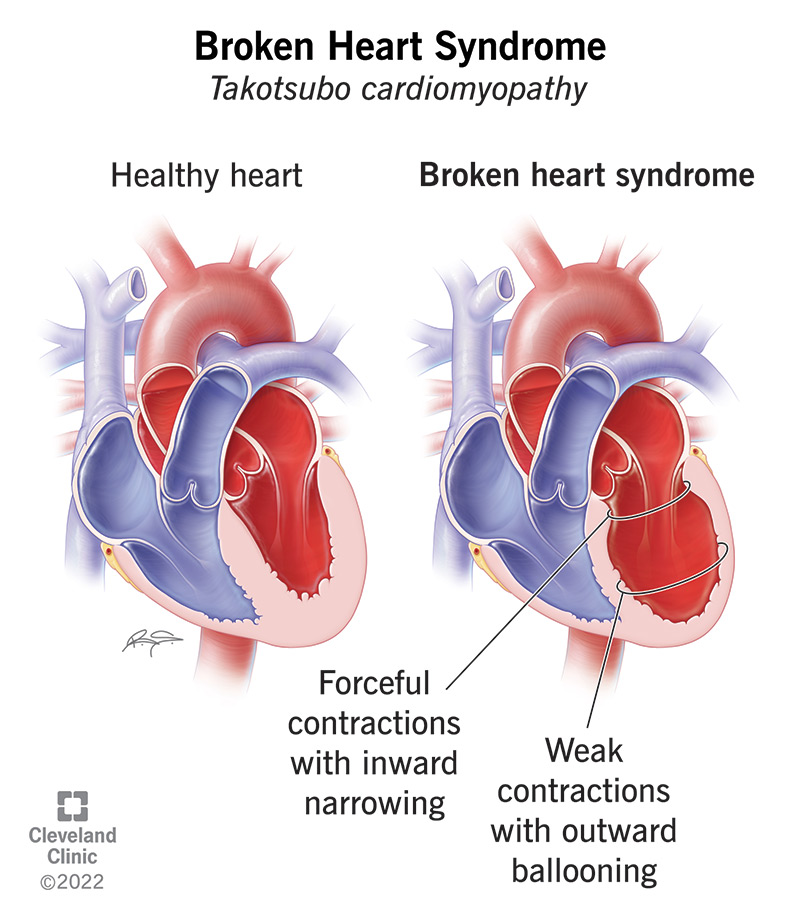
The relationship between severe emotional stress and heart health is not recent. The medical community has long recognized a phenomenon often called broken heart syndrome
(Takotsubo cardiomyopathy), where extreme stress triggers a sudden weakening of the left ventricle. However, bereavement-related risk extends beyond this acute condition to long-term cardiovascular instability.
When a person experiences a profound loss, the body’s stress response system goes into overdrive. This involves the release of catecholamines (like adrenaline) and the activation of the hypothalamic-pituitary-adrenal (HPA) axis, which increases cortisol levels. Over time, this chronic stress state can lead to:
- Increased Blood Pressure: Persistent stress keeps the body in a “fight or flight” mode, raising blood pressure and straining arterial walls.
- Inflammation: Grief can trigger systemic inflammation, a known driver of atherosclerosis (the buildup of plaques in the arteries).
- Behavioral Shifts: Bereavement often leads to poor sleep, decreased physical activity and neglected medication adherence, all of which exacerbate heart risk.
The COVID-19 Pandemic: A Catalyst for Risk
While bereavement has always been a risk factor for heart disease, the COVID-19 pandemic introduced unique stressors that amplified this vulnerability. According to a cohort study highlighted by Mirage News and based on data from the JAMA Network, the association between loss and cardiovascular risk was notably stronger during the pandemic, particularly regarding the loss of a partner or sibling.
Several factors likely contributed to this heightened risk during the pandemic era:
- Isolated Grief: Social distancing and lockdowns prevented traditional mourning rituals and support systems, leaving many to process grief in isolation.
- Compounded Stress: The loss of a loved one often occurred alongside financial instability and a general atmosphere of global health anxiety.
- Healthcare Disruptions: Many bereaved individuals delayed routine cardiovascular screenings or management of chronic conditions due to pandemic-related clinic closures.
Who is Most at Risk?
Not all bereavement experiences impact the heart in the same way. Research suggests that the closeness of the relationship is a primary driver of risk. The loss of a spouse or partner typically carries the highest risk for acute cardiovascular events, as it often involves the loss of a primary emotional support system and a significant shift in daily living habits.
Age and pre-existing conditions also play a role. Individuals who already have hypertension, diabetes, or a history of coronary artery disease are more susceptible to the physiological “shock” of bereavement, making them high-priority candidates for clinical monitoring during the grieving process.
- Bereavement is associated with an increased risk of cardiovascular disease both before and during the COVID-19 pandemic.
- The risk is particularly acute following the loss of a partner or sibling.
- Physiological triggers include chronic inflammation and the overactivation of the body’s stress response.
- Clinical monitoring and preventive care are essential for bereaved individuals to mitigate heart risks.
Managing Cardiovascular Health During Grief
Since the period following a loss is a time of heightened vulnerability, a proactive approach to health is vital. If you or a loved one are grieving, consider these evidence-based strategies to protect heart health:
1. Prioritize Clinical Check-ups
Don’t ignore “minor” symptoms. Chest pain, shortness of breath, or unusual fatigue during a period of grief should be evaluated by a physician immediately to rule out acute cardiac events.
2. Maintain Medication Adherence
It’s common to forget medications during the “brain fog” of grief. Use pill organizers or phone alerts to ensure that blood pressure and cholesterol medications are taken consistently.
3. Seek Integrated Support
Psychological support is physical support. Therapy and support groups can assist lower the chronic stress load on the body, potentially reducing the inflammatory response associated with grief.
Frequently Asked Questions
Does the risk of heart disease decrease after the initial period of grief?
While the risk for acute events is highest shortly after the loss, the long-term impact depends on the individual’s ability to adapt and their access to support. Chronic grief can lead to sustained cardiovascular strain if not managed.
Is “Broken Heart Syndrome” the same as a heart attack?
No. While both can cause chest pain and shortness of breath, a heart attack is typically caused by a blocked artery. Broken Heart Syndrome (Takotsubo cardiomyopathy) is a temporary weakening of the heart muscle triggered by severe stress, though it can still be life-threatening.
Can exercise help mitigate bereavement-related heart risk?
Yes. Gentle physical activity, such as walking, can help regulate blood pressure and improve mood, which in turn lowers the stress hormones that damage the heart. However, those with pre-existing conditions should consult a doctor before starting a new regimen.
As we move further away from the peak of the pandemic, the lessons learned from this period emphasize a holistic approach to medicine. Treating the heart requires more than just managing lipids and blood pressure; it requires acknowledging the profound impact of emotional trauma on physical health.