Sleep isn’t just a period of downtime; it’s a critical biological process that allows the brain to flush out toxins, consolidate memories, and repair cellular damage. When this process is interrupted by a sleep disorder, the consequences ripple through every aspect of health, from cognitive function and emotional stability to cardiovascular wellness. Understanding the specific nature of these disruptions is the first step toward reclaiming restorative rest.
- Sleep disorders are categorized by symptoms such as difficulty falling asleep, excessive daytime sleepiness, or abnormal movements during sleep.
- Common conditions include insomnia, sleep apnea, and narcolepsy.
- Movement disorders, like Restless Legs Syndrome (RLS), can significantly degrade sleep quality.
- Most sleep disorders are treatable through a combination of lifestyle changes, cognitive behavioral therapy, and medical intervention.
Common Types of Sleep Disorders
Sleep disorders are diverse, ranging from behavioral issues to complex neurological malfunctions. They are generally grouped by the primary symptom they produce.
Insomnia
Insomnia is the most prevalent sleep disorder. It isn’t just “not being able to sleep”; it’s a persistent difficulty with sleep initiation, maintenance, or quality, despite having the opportunity for sleep. Insomnia can be acute (short-term) or chronic, often triggered by stress, anxiety, or poor sleep hygiene.
Sleep Apnea
Sleep apnea involves repeated interruptions in breathing during sleep. The most common form, Obstructive Sleep Apnea (OSA), occurs when throat muscles relax and block the airway. This forces the brain to briefly wake the person up to resume breathing, often resulting in loud snoring and severe daytime fatigue. According to the Mayo Clinic, untreated sleep apnea increases the risk of hypertension and heart disease.
Narcolepsy
Narcolepsy is a neurological disorder that affects the brain’s ability to control sleep-wake cycles. People with narcolepsy experience excessive daytime sleepiness and “sleep attacks”—sudden, irresistible urges to sleep. Some also experience cataplexy, a sudden loss of muscle tone triggered by strong emotions.
The Intersection of Movement and Sleep
Certain disorders manifest as physical movements that disrupt the sleep cycle. These “sleep-related movement disorders” can prevent a person from reaching the deep, restorative stages of sleep.
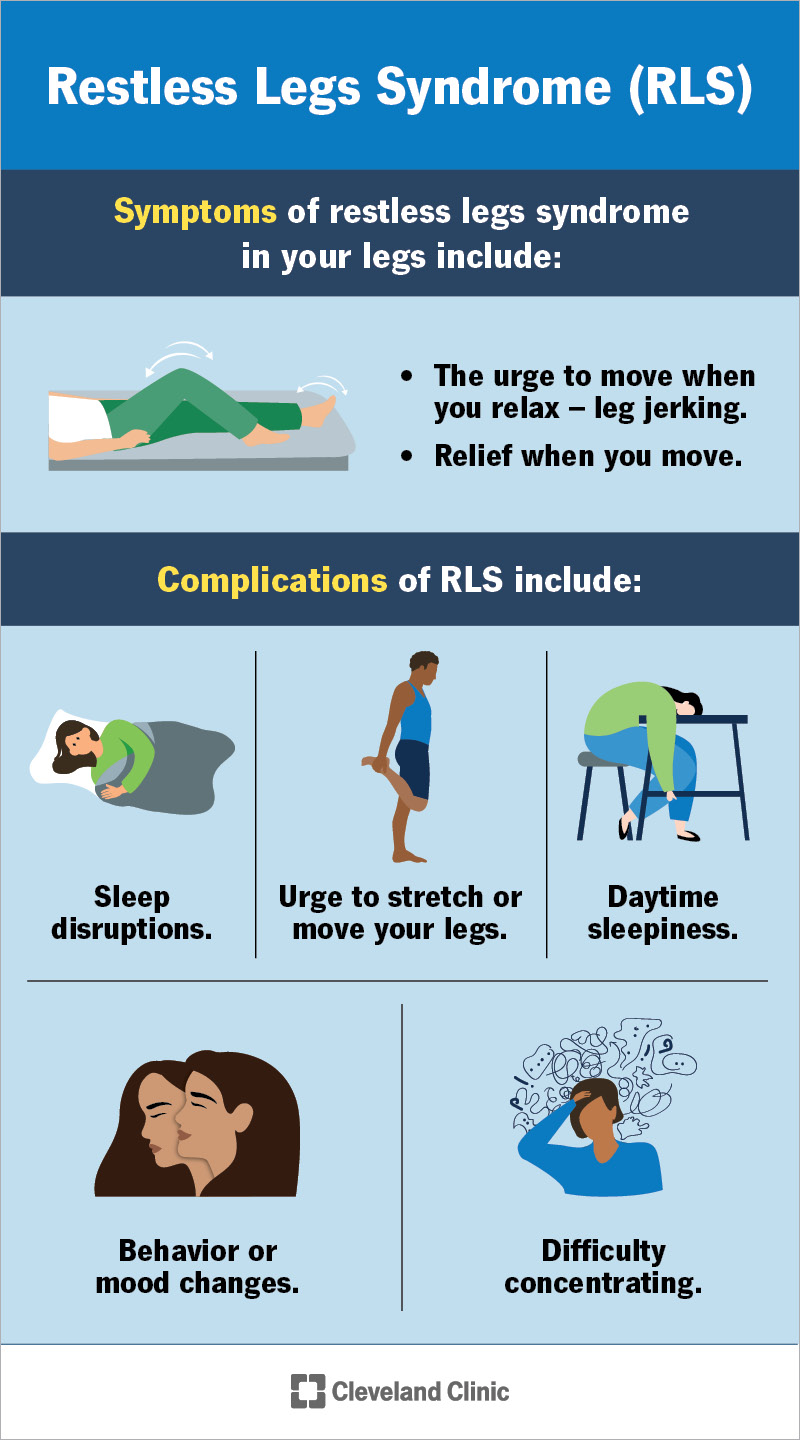
Restless Legs Syndrome (RLS)
RLS is characterized by an irresistible urge to move the legs, usually accompanied by uncomfortable sensations (like tingling or crawling) that worsen during periods of rest. This often prevents the onset of sleep and leads to fragmented rest.
Periodic Limb Movement Disorder (PLMD)
Unlike RLS, which occurs while awake, PLMD involves repetitive cramping or jerking of the legs during sleep. While the sleeper may not remember these movements, they often wake up feeling unrefreshed because the movements trigger “micro-arousals” that disrupt the sleep architecture.
The Impact of Poor Sleep on Overall Health
Chronic sleep deprivation doesn’t just make you tired; it actively degrades your physiological systems. When you don’t get enough quality sleep, your body remains in a state of stress.
- Cognitive Decline: Lack of sleep impairs attention, executive function, and decision-making capabilities.
- Metabolic Disruption: Sleep loss affects the hormones that regulate hunger (leptin and ghrelin), often leading to weight gain and an increased risk of type 2 diabetes.
- Mental Health: There is a bidirectional relationship between sleep and mental health; insomnia can trigger depression and anxiety, and vice versa.
- Immune Suppression: During sleep, the immune system releases proteins called cytokines. Insufficient sleep reduces the production of these protective proteins, making you more susceptible to infections.
Diagnosis and Treatment Strategies
Treating a sleep disorder requires an accurate diagnosis to ensure the intervention matches the cause. A physician may recommend a polysomnography (sleep study), where brain waves, oxygen levels, heart rate, and breathing are monitored overnight.
Evidence-Based Treatments
Depending on the diagnosis, treatment typically follows these paths:
- Cognitive Behavioral Therapy for Insomnia (CBT-I): Considered the gold standard for chronic insomnia, CBT-I addresses the thoughts and behaviors that keep people awake.
- CPAP Therapy: Continuous Positive Airway Pressure (CPAP) machines are the primary treatment for obstructive sleep apnea, using air pressure to keep the airway open.
- Pharmacological Intervention: In some cases, medications may be used to manage symptoms of narcolepsy or RLS, though these are typically secondary to behavioral changes.
- Sleep Hygiene Optimization: This involves creating a strict sleep schedule, limiting caffeine and alcohol, and ensuring the bedroom is dark, cool, and quiet.
Frequently Asked Questions
Can stress cause a permanent sleep disorder?
Stress usually causes acute insomnia. However, if a person develops a “fear of not sleeping,” it can create a psychological loop that turns a temporary problem into a chronic sleep disorder. Early intervention with a healthcare provider is key to preventing this transition.

Is snoring always a sign of sleep apnea?
No, snoring is common and doesn’t always indicate a disorder. However, if snoring is accompanied by gasping for air, choking sounds, or extreme daytime sleepiness, it is a strong indicator of sleep apnea and requires medical evaluation.
How much sleep do adults actually need?
While individual needs vary, most adults require between 7 and 9 hours of quality sleep per night to maintain optimal health and cognitive function.
Looking Ahead
The field of sleep medicine is rapidly evolving, with new research focusing on the role of the glymphatic system—the brain’s waste-clearance system—and how specific sleep stages impact long-term neurological health. As we move toward more personalized medicine, treatments are becoming more tailored to an individual’s genetic makeup and circadian rhythm, promising a future where restorative sleep is accessible to everyone.